Arthroscopy changed orthopedic surgery in the same way laparoscopy changed general surgery. The same operations that used to need a 15-centimetre incision and a 5-day hospital stay are now done through three or four small punctures, with same-day or next-morning discharge. Pain is less. Scarring is minimal. Recovery is faster.
Dr. Swaroop Solunke runs an active arthroscopy practice at his Wakad clinic and partner hospitals across PCMC. The two joints arthroscopy is most often used for are the knee and the shoulder - they are also the two joints most often injured by IT professionals, weekend athletes and active homemakers across Pune.
What Is Arthroscopy?
Arthroscopy uses a thin tube with a camera at its tip (the arthroscope) inserted through a small incision in the skin. The camera sends a magnified image to a high-definition monitor. Through one or two more small incisions, the surgeon inserts specialized instruments to repair, trim, reattach or reconstruct tissue inside the joint.
Because the incisions are small (4 to 8 millimetres each), there is far less tissue trauma than open surgery. Bleeding is minimal. Hospital stay is short. Most arthroscopic procedures are done as day-care surgery - the patient walks out of the hospital the same evening.
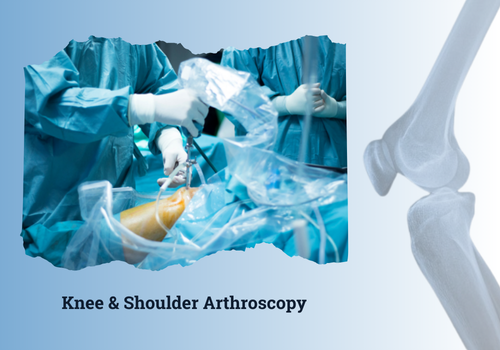
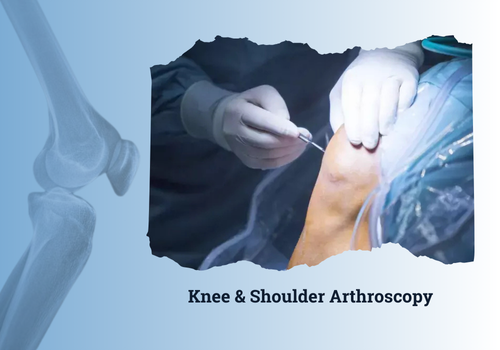
Knee Arthroscopy - Conditions Treated
ACL (Anterior Cruciate Ligament) Tear
The most commonly torn knee ligament. Usually happens in cricket, football, badminton or basketball - also in road accidents and falls. ACL reconstruction is done arthroscopically using a graft from the patient's hamstring or patellar tendon.
Meniscus Tear
The meniscus is a C-shaped cartilage cushion between the thigh bone and shin bone. Tears happen from twisting injuries, deep squats or with age. Arthroscopy lets the surgeon either repair the tear (preferred when possible) or trim the damaged portion.
Cartilage Damage
Loose cartilage flaps are trimmed. Areas of damaged cartilage may be treated with microfracture, chondroplasty or cartilage-restoration techniques.
Patellar (Kneecap) Problems
Recurrent kneecap dislocation, patellar tendon issues and chondromalacia patellae can all be treated arthroscopically.
Loose Bodies
Free-floating bone or cartilage fragments that cause locking and catching are removed.
Shoulder Arthroscopy - Conditions Treated
Rotator Cuff Tear
The rotator cuff is a group of four tendons that stabilize and move the shoulder. Tears cause weakness, pain at night and difficulty lifting the arm overhead. Arthroscopic rotator cuff repair reattaches the torn tendon to bone using anchors.
Shoulder Dislocation and Instability (Bankart Lesion)
Repeated shoulder dislocations, common in young athletes, are caused by tearing of the labrum (Bankart lesion). Arthroscopic Bankart repair re-secures the labrum using suture anchors.
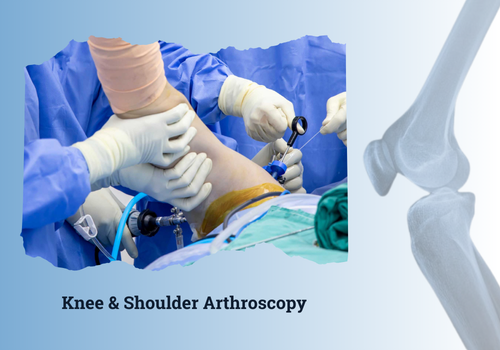
SLAP Tear
A tear of the labrum at the top of the shoulder socket. Often seen in throwing athletes and patients with biceps tendon problems.
Frozen Shoulder (Adhesive Capsulitis)
When physiotherapy and injections are not enough, arthroscopic capsular release frees the stiff joint.
Subacromial Impingement
Bone spurs at the top of the shoulder pinch the rotator cuff. Arthroscopic acromioplasty removes the spur.
How Arthroscopy Is Performed
Most arthroscopies are done under regional anesthesia or general anesthesia. The surgery typically takes 45 to 90 minutes depending on what is being treated.
Three small incisions are made around the joint. Sterile fluid is pumped in to expand the joint and improve visibility. The arthroscope goes through one portal; instruments through the others. The surgeon watches a high-definition monitor and works inside the joint with millimetre precision.
After the procedure, incisions are closed with one or two stitches each (sometimes just adhesive strips). A sling or brace is applied if needed.
Pricing for Arthroscopic Surgery
- Diagnostic knee arthroscopy: Rs. 60,000 to Rs. 90,000
- Meniscus repair or trimming: Rs. 80,000 to Rs. 1.4 lakh
- ACL reconstruction: Rs. 1.2 to 2 lakh
- Rotator cuff repair: Rs. 1.5 to 2.5 lakh
- Bankart repair (shoulder stabilization): Rs. 1.4 to 2.2 lakh
- Shoulder capsular release for frozen shoulder: Rs. 1 to 1.5 lakh
All arthroscopic surgeries are typically day-care or 24-hour stay procedures. Mediclaim is widely accepted.
Recovery After Arthroscopic Surgery
Day 1 to 7
Rest, ice, elevation. Pain is usually well-controlled with oral medication. Knee patients walk with crutches; shoulder patients wear a sling. Stitches removed at day 10 to 14.
Week 2 to 6
Structured physiotherapy begins. Range of motion is restored first, then strength.
Week 6 to 12
Most desk-job patients are fully back to work. Light gym and swimming permitted.
Month 3 to 6
Return to sports. ACL reconstruction patients return to non-contact sports at month 4 to 5 and contact sports at month 6 to 9.
Linked Treatment Pages
- Knee Arthroscopy / Arthroscopic Knee Surgery
- Shoulder Arthroscopy and Bankart Repair
- ACL Reconstruction Surgery
- Sports Injury Surgery and Treatment